Removing complex teeth safely and with minimal impact.
This chronic feline oral disease is a commonly occurring, complex syndrome. It is characterised by often severe, debilitating and protracted oral inflammation in cats. The cause of the condition remains unknown and may be multifactorial. It is clear that cats with feline chronic gingivostomatitis have an inappropriate immune response to an inciting trigger. The specific trigger or triggers may be different amongst cats.

Potential causes
Several potential causes or triggers for feline chronic gingivostomatitis have been suggested, including viruses (feline calicivirus, herpesvirus, leukemia virus, immunodeficiency virus), bacteria (bartonella), dental disease (tooth resorption, periodontal disease), and hypersensitivity reactions (overreaction to plaque bacteria, food allergies). It’s possible that some or all of these factors may trigger an immune response in individual cats.
Cats with this condition experience moderate to severe oral pain, which may lead to reduced appetite or changes in food preferences, often favouring softer items. They may resent being handled, especially around the mouth, paw at their mouth, drool excessively, have difficulty swallowing and become irritable or withdrawn, leading to weight loss. These symptoms make oral examination challenging and can complicate treatment regimens that require administering medication by mouth.
“When every meal becomes painful, compassionate dental treatment can give cats with FCGS a chance to enjoy life again.”
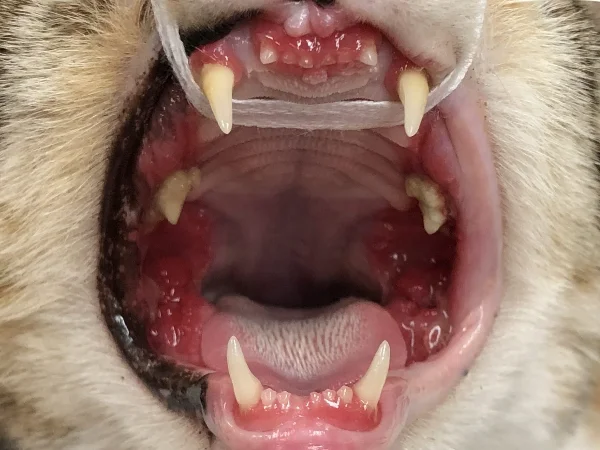
Differentiating Feline Chronic Gingivostomatitis
Feline chronic gingivostomatitis differs from gingivitis when inflammation extends beyond the gums to include the buccal mucosa (cheeks) and soft tissue at the back of the mouth, lateral to the palatoglossal folds—often mistakenly called the “fauces.”
In this condition, not only are the gums inflamed, but the adjacent mucosa is as well. The affected tissue is friable, bleeds easily upon palpation, and often presents with proliferative or ulcerative lesions.
Feline chronic gingivostomatitis seems to be more common in purebred cats, those living in multi-cat households, and cats in shelter environments.
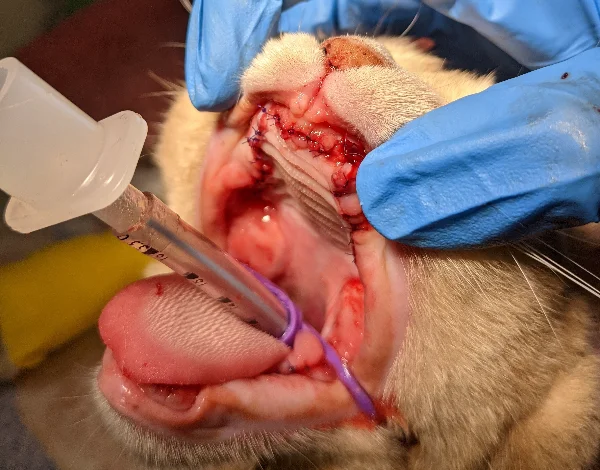
Treatment
A consistently successful treatment option has yet to be determined. Numerous different approaches to treatment have been trialled over many years, with surgical treatment being considered the most consistently successful and appropriate at present.
Surgical treatment involves either full mouth extractions or extraction of all premolar and molar teeth (those behind the canine teeth). The precise reason aggressive extraction of teeth is successful in so many patients is not entirely understood.
Our expectation is that approximately 70-80% of patients treated with caudal or full mouth extractions will have resolution of their feline chronic gingivostomatitis symptoms. For many, this is a complete cure, whilst for some, the use of medical management is still required intermittently. Sadly 20-30% of patients unfortunately fail to show any improvement following surgical treatment.
Extractions must be performed by skilled professionals using dental radiology to ensure complete removal of all tooth material. Any remaining tooth material is a common cause of surgical treatment failure.
“FCGS is overwhelming for many cats — but early diagnosis and the right care can dramatically restore comfort and wellbeing.”

Medical Therapy & Supportive Care
Many medical therapies for gingivostomatitis focus on immune suppression, with corticosteroids and cyclosporine being the most commonly used.
However, these treatments often carry significant side effects, tend to lose effectiveness over time, and rarely provide long-term resolution.
Medical management should be considered only as a supplementary approach for patients who haven’t fully responded to surgical treatment.
Cats testing positive for feline immunodeficiency virus (FIV) are less likely to respond favourably to treatment, making FIV testing crucial for all feline chronic gingivostomatitis cases to inform prognosis.
However, some FIV-positive patients do respond well to treatment.
Supportive care is vital, as many patients endure moderate to severe oral pain. Proper pain management, nutritional support, grooming assistance and sometimes antibiotic therapy are essential for managing symptoms before and after extractions, particularly for those who haven’t fully responded to treatment.
Sadly, some patients do not respond adequately to any form of treatment, and in severe cases, euthanasia may be considered due to the significant impact on their quality of life.
Prevention
Until the cause of feline chronic gingivostomatitis is clearly understood, no prevention is possible. Research is ongoing into potential causes and more effective treatment options. There have been some positive results from recent trials being conducted with stem cell therapy, this may offer hope for a more reliable and less invasive treatment options to patients in the future.














