Removing complex teeth safely and with minimal impact.
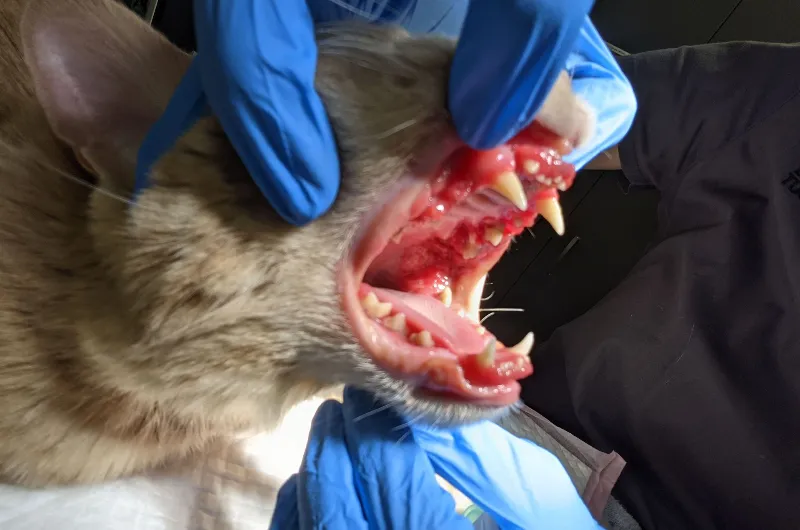
Some conditions are just difficult, no matter how often you encounter them. Feline chronic gingivostomatitis (FCGS) is one of them. It’s not rare; most vets will have managed more than one case, but it is unpredictable. Two cats can present in almost the same way, follow a similar treatment plan, and then still end up with completely different outcomes. That variability is what makes this condition challenging and influences how it is approached in practice.
At Advanced Animal Dentistry, we treat complex dental disease in pets in Brisbane and the Gold Coast, including FCGS. Our focus is always on making informed decisions at the right time, based on what is in front of us rather than following a fixed plan.
“Two cats can present similarly, follow the same treatment plans, and still have completely different outcomes.”
Why cases vary significantly
One of the ongoing limitations in managing FCGS is that there is still no single, clearly defined cause. The etiology of FCGS remains elusive, but it is generally accepted that FCGS arises from an inappropriate immune response to oral antigenic stimulation, potentially multifactorial in nature and possibly with varying inciting causes. Importantly, FCGS differs from more common dental conditions such as gingivitis, where inflammation is typically limited to the periodontal tissues. In FCGS, the inflammatory process extends beyond these structures into the oral mucosal surfaces, which is a key feature in identifying affected cases.
A number of factors have been linked to the condition and may contribute to inflammation, including:
- Viral involvement, particularly feline calicivirus and other infectious agents
- Changes in the oral microbiome, including shifts in bacterial populations
This is why feline chronic gingivostomatitis is thought by many to be multifactorial. While we do not know this for sure, in many cases, it seems not to be a single trigger, but a combination of contributing factors.
The severity of FCGS
It really is a horrible disease and, outside of oral cancer, it is one of the few dental conditions that can lead to discussions about euthanasia. That comes down to the level of pain involved. It’s not just inflammation seen on an exam; it affects how a cat functions day to day. Some reach a point where eating becomes difficult or even impossible. They may approach food, try to eat, then vocalise and pull away. Others stop eating altogether.
But just as there may be a spectrum of triggers, there’s also a spectrum in how it presents. Some cats have a mouth that looks severe but are coping relatively well, while others show less obvious changes, yet are much more affected clinically.
FCGS is not static. It can fluctuate within the same patient, with periods of improvement followed by deterioration. That makes it difficult to judge progression or response, because what you see at a single point in time may not reflect the overall pattern.
This is what sets FCGS apart from more routine dental conditions. Assessment extends beyond what can be seen on examination, and requires consideration of how the disease is affecting the patient more broadly.
“Feline chronic gingivostomatitis is often multifactorial, not driven by a single cause.”
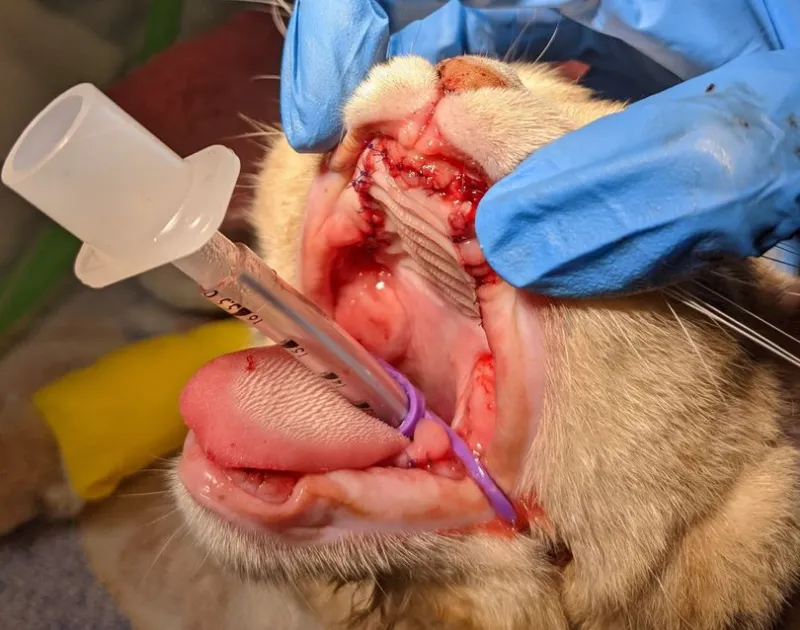
Current approaches to treatment
Presently, dental extractions have the strongest body of evidence behind them and remain the most reliable option for achieving remission in FCGS. While full mouth or near full mouth extractions will not cure every patient, the literature shows a high proportion improve, which aligns with what we see in practice.
However, there are no guarantees. Some cats do very well, some improve but continue to require support, and some show little change. Technique can also influence outcomes. A cat that has undergone full mouth extractions but still has retained roots or residual dental material is not in the same position as one where removal has been thorough. In those cases, the result may be limited, or the patient may remain uncomfortable.
This likely contributes to the ongoing debate around extractions, with some viewing them as too aggressive. It’s not an unreasonable concern. Full mouth extractions are significant procedures; they are costly, and they don’t come with any assurances. That said, when they are successful, the change can be profound. Some cats improve dramatically, while others may still require ongoing management.
Medical management is also often part of the treatment plan. A range of therapies have been trialled, including corticosteroids, cyclosporine, interferon, lactoferrin and stem cell therapy, with mixed results across studies. In practice, some options can work very well for one cat and have little effect on another. These treatments have a role, but at this stage, they have not shown the same consistency in achieving remission as extractions. Also important to note, many of these treatments are often used after extractions and are rarely sufficient on their own.
These medications are not benign. Some come with significant complications, and over time they can also become expensive. That matters because many cats do not move quickly to a more definitive plan. Instead, they can spend months, sometimes much longer, moving from one option to the next before referral or a more decisive intervention is considered.
With multiple options and no clear guarantees, it’s understandable that treatment planning for FCGS can become complex.
Developments in treatment and what to consider
There has been growing interest in newer options for treating FCGS, including antiviral therapies targeting feline calicivirus. Given there is evidence it may play a role in some cases, this is a reasonable line of investigation. While we are optimistic about these developments and do use them where appropriate, they need to be approached with care.
At this stage, structured clinical data remains limited. There is a lack of controlled trials and standardised ways to confirm diagnosis or assess response, which makes outcomes difficult to interpret. There is also a broader consideration around how quickly new therapies are being adopted in practice, particularly when supporting data is not yet well established.
Additionally, even when medical therapy is effective, many cats with FCGS still have concurrent dental disease, such as resorption or periodontal disease. These can persist independently and continue to cause pain if not addressed, which is why treatment needs to consider the mouth as a whole.
There are also practical considerations. Many of these newer therapies are used off-label, with limited prescribing guidance. In these situations, responsibility remains with the prescribing veterinarian, along with careful case selection, monitoring and clear communication with owners.
“Extractions remain the most reliable option, but they do not come with guarantees.”
Navigating a complex condition
There is hope for a future where FCGS can be managed more effectively and with less reliance on invasive treatment, but for now, medical options sit alongside surgical extractions rather than replacing them. It remains a difficult diagnosis to deliver to cat families, and the approach to care should always reflect the individual patient and what they need.
Ultimately, we still don’t fully understand this disease and its cause or causes, and that’s why there is no single, reliable solution. In some respects, it may be more accurate to think of FCGS as a syndrome rather than a single disease.
If you’d like to know more about FCGS and treatment options, contact our friendly team today.
To refer a patient to Advanced Animal Dentistry, complete the referral form here.













